Team care is changing the way clinics work and the way they’re designed. Here’s how it’s improving throughput, efficiency and relationships between patients and staff.
In 2012, a physician at the Cleveland Clinic tried something new to cope with increasing patient volumes and changes in reimbursement. The goal was to improve efficiency, maintain quality patient care, and boost patient and staff satisfaction. Dr. Kevin Hopkins began working alongside his staff in a [reconfigured] environment, and it didn’t take long to see significant benefits: an increase in the number of patients he saw each day, a 23 percent jump in gross patient revenue, and much happier staff and patients. Hopkins had discovered the power of the team care model, an emerging trend that’s improving patient services through redesigned clinic layouts.
Changing dynamics in healthcare
With the implementation of the Affordable Care Act, outpatient clinics across the country are being forced to rethink how they manage all this new activity. That’s not the only driver of change; consumers today also expect a better medical experience, and are more selective of where they choose to receive care, often choosing the easiest, in-and-out options available to them.
So providers are striving to increase patient satisfaction through shorter wait times, better accessibility and interaction, and a sense of patient empowerment – all key motivators to keep people returning. This has led to a reevaluation of the standard clinic model, in which physicians typically had a private office separated from a nurses station or exam rooms for privacy.
Like Dr. Hopkins, many physicians are implementing team care, a more collaborative model of patient care. Team care allows for greater interaction between patients and providers, and between providers themselves, by using time and resources more efficiently. Team care uses flexible staff workspaces, new treatment modalities, and a renewed focus on patient satisfaction.
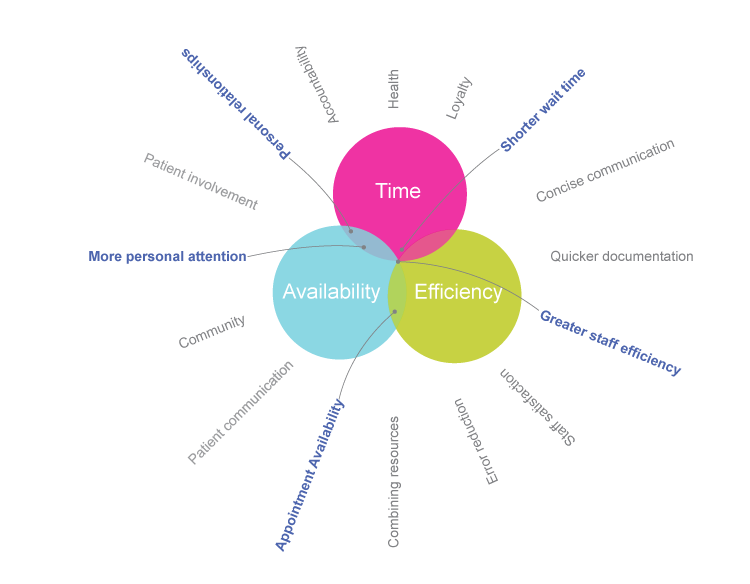
Rethinking space to create efficiencies
At the core of team care is a unified, collaborative clinic configuration: all providers, whether they’re physicians, nurses or physicians assistants, work side by side in closer proximity while providing patient care. This can happen in a shared office where PA, MAs, or RNs work alongside physicians, or in an office shared with other providers. This method has been shown to increase efficiency and communication, improve the patients’ experience and the quality of their visit, and even lower the number of hospital admissions by resulting in healthier, happier patients.
Traditionally, a semi-private space gave physicians a quiet area to chart and perform other administrative tasks, and private offices kept them further away from the action. The team care alternative to this is to provide larger, open work areas that are centrally located and surrounded by exam rooms and support space shared by multiple physician/support teams. This reduces the distance traveled between the workstation and an exam room, saving time.
Proponents of this concept stress a greater ability for staff to assist when needed, and easier information sharing. To maximize collaboration and efficiency without distraction, research has suggested that the maximum number of providers in one workspace be limited to two teams.
Essentially this plan creates spaces, or “pods,” which can be replicated, using shared support spaces in between to allow for flexibility among multiple pods to accommodate more providers and exam rooms. Along with the implementation of larger, more communal workspaces, it’s important to include open offices that can be used by staff for patient, financial, or specialist consults, or to perform other quiet tasks where an open workstation is not preferred. The goal is to be able to facilitate all of a patient’s needs within one space and one visit, bringing the clinician to the patient to help guarantee the patient is following up on their recommended care.
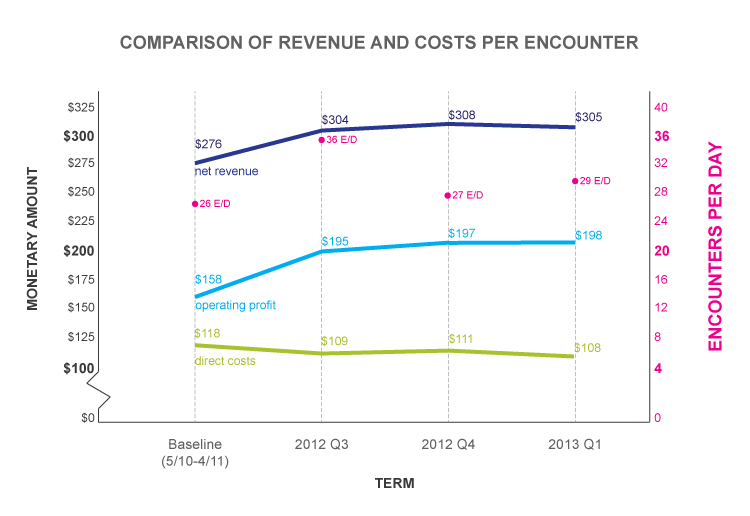
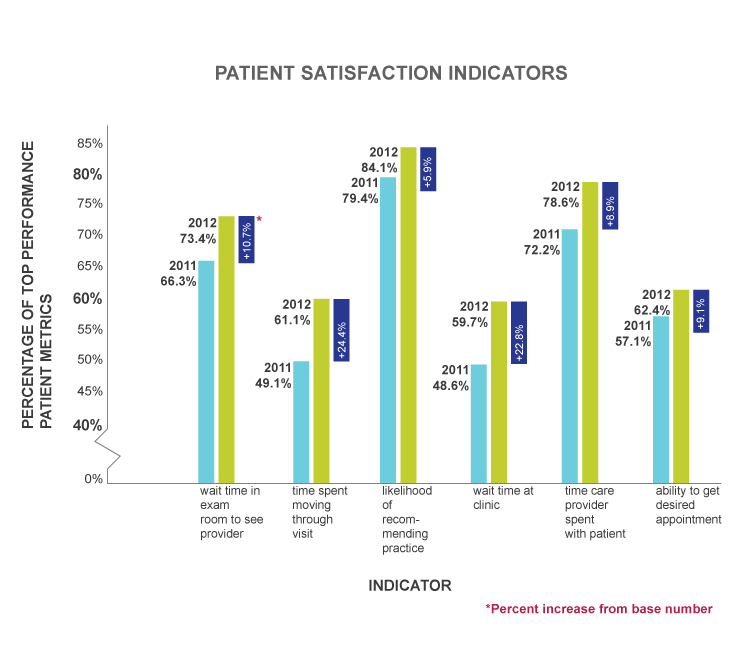
After experiencing the team care model at the Cleveland Clinic, Dr. Hopkins’ patients reported higher satisfaction with their wait times, the time spent with the physician or staff members, and the ease of scheduling appointments, among other measures.
Planning the team care space
Traditionally, physicians have kept private offices within a practice and the much of the remainder of the clinic staff worked together in a larger group work area or utilized separate charting stations within or outside of exam rooms. Support space and exam rooms have typically surrounded a group work area, thus reducing the steps for most of the staff while the physician’s offices were often separate from the exam rooms to create privacy. This model is exactly the workflow that Dr. Hopkins was striving to change and make more efficient.
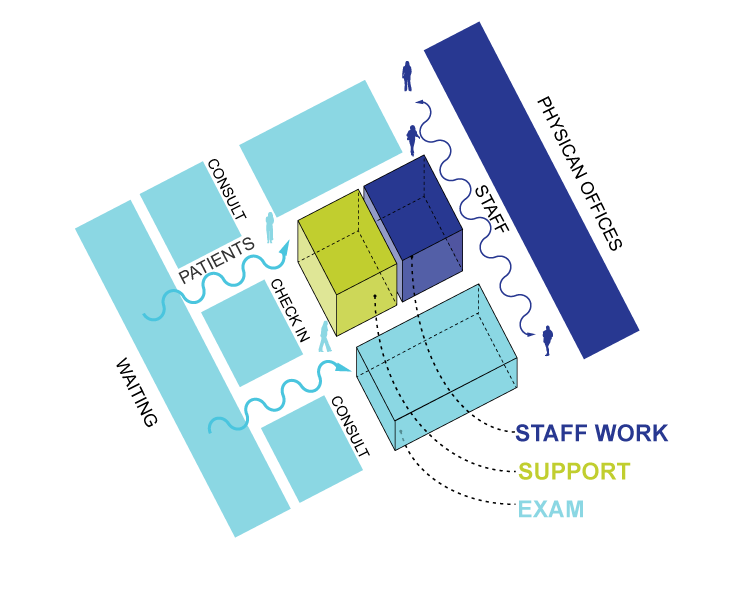
There are a number of ways healthcare groups have adapted their spaces to the team care model. Variations reflect surrounding demographics and patient populations. When implemented, these care models have different implications on the overall planning and layout of future clinics. One approach to the team care model is the on-stage/off-stage method, which separates the more public areas from the private, behind-the-scenes work and staff areas with dual access to patient rooms. Staff areas on the interior are grouped together into pods with support functions to allow for greater collaboration and to keep these functions accessible to the staff but not visible to the patients.
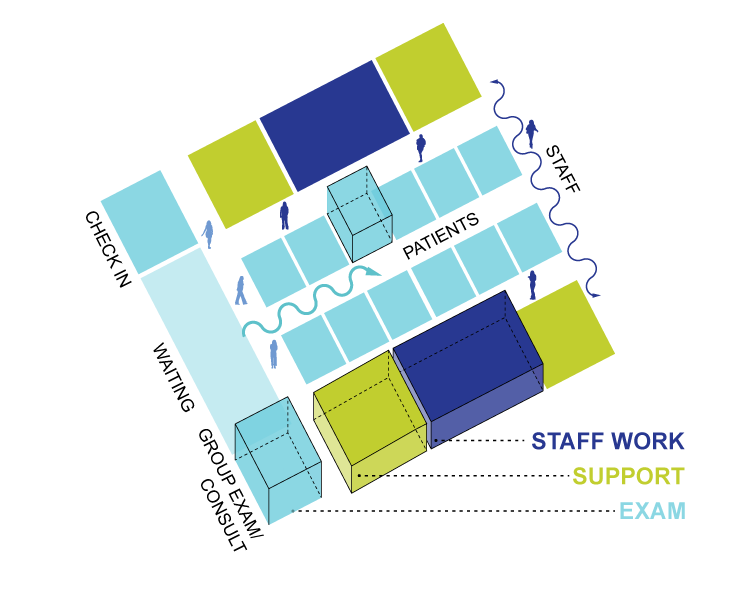
Another variation, the self-rooming method, allows patients to check themselves in and go directly to their exam rooms, sometimes with the help of a tracking device. Self-rooming is designed to give providers a workspace near their group of exam rooms, allowing them to chart immediately after seeing a patient that in turn allows them spend more time with patients.
The physician and staff collaborative is yet another option. This approach emphasizes the need for semi-private spaces in close proximity to open workstations, allowing for collaboration and quiet when both are needed. These clinics are often set up with a traditional check-in/check-out, with the exam space broken down into nurse stations in close proximity to shared physician offices and surrounded by their designated exam rooms.
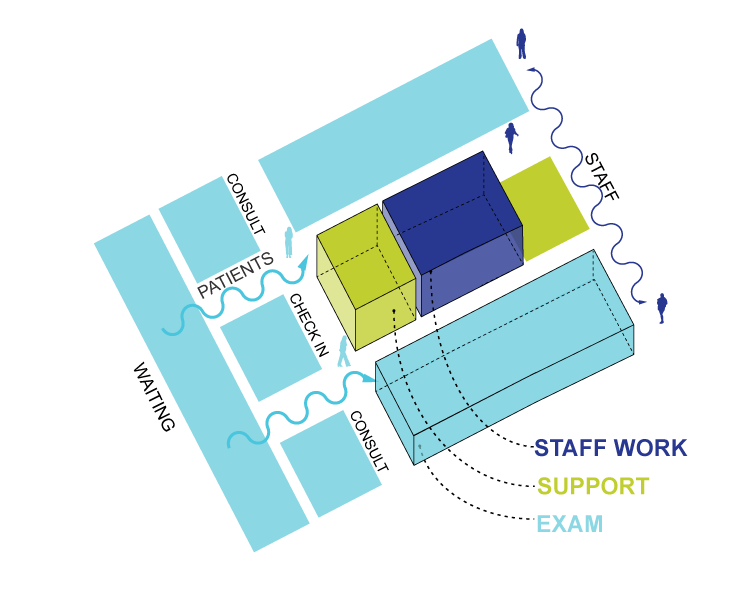
Each of these models incorporate shared collaboration spaces but also include open offices, ideally the dimension of an exam room for possible future expansion, for use by all staff and patients. Yet it’s also important to keep these pod sizes small to allow for a concentration on the patients and ease of access to supplies and exam rooms. If possible, staff workspaces should be flexible to allow for multiple types of staff-to-staff and patient-to-staff interactions.
Furniture companies have been developing their own versions of multi-faceted workstations which allow for seated or standing work height, a variety of different desktop configurations, and ease of reconfiguration for future changes to work practices. While the aim of the team care model is to create better patient-staff relationships and increase productivity, this model also has the ability to create plan efficiencies and reduce the amount of space required for work areas by up to 50 percent.
Clinics of the future
Technology is also playing an important role in the next-generation clinic. Some healthcare groups are using self-check-in kiosks to minimize waiting time while others are using tablets in their waiting rooms to help sign patients in and get them roomed more quickly. The tablet also has the potential for sharing wellness videos and information with patients, even helping communicate with providers in other locations. Another use for tablets: Increasingly, they’re being used by providers in place of the traditional workstation on wheels or desktop workstation, providing more freedom and the ability to work in multiple environments.
In the clinic of the future it’s important to recognize that changing technology, and changing perceptions and methods of delivering healthcare, will quickly alter our thoughts on clinic planning. The more flexibility that’s built into a space — whether that be through consistently dimensioned modules or prototypes, the ability to easily reconfigure spaces or the accommodation of many different forms of technology — the easier it will be for each clinic to provide cutting edge, quality care for their patients.

Anna Kalnow, NCIDQ, LEED AP BD+C // Interior Designer
As a skillful designer, Anna understands the needs of patients, their families and staff as well as the operational implications of the healthcare environment. While leading the development of concepts, she translates the design criteria, image development and innovative solutions. She is passionate about the power and need of interior design to create healthy and healing environments.
Anna has recently been working with The Cleveland Clinic to evaluate space and work efficiencies to help develop best practices relating to clinical design and patient satisfaction.
