Complex healthcare situations rely on well-educated professionals. And the best medical education facilities have these three things in common. For Education Market lead Ben Niebauer, getting it right is personal.
By: Ben Niebauer, RA, LEED AP BD+C // Associate Principal, Education Market Leader
In the waning hours of an otherwise average Saturday in the Spring of 2019, my daughter fell while playing with friends and broke not one, but BOTH of her arms. The injuries resulted in a trip to an emergency room, surgery on one of the arms, an overnight stay at the hospital, follow-up outpatient procedures, and about six months of physical therapy.
It’s been a year and a half since the event, and, thankfully, my daughter once again has two fully functioning arms. When it happened, my singular focus was on helping my child: getting her to the right healthcare professionals. Looking back on the experience, I’m struck by just how many of them helped us in our relatively short experience.
Not counting receptionists, administrators, or other staff, I remember dealing with at least 24 different nurses, aides, doctors, pharmacists or physical therapists in the process. And this statistic doesn’t include all of the people we didn’t see or directly engage: those who assisted in surgery, developed x-rays, or otherwise supported the efforts of the front-line professionals with whom we interacted.
More than just the skill of any one individual, it was the collaborative, coordinated effort of this extended team that led to my daughter’s successful recovery. Where do these professionals learn to choreograph this collaboration? Simply put, they start in school, in the types of spaces I help design. All 24 of those professionals went to a university for between two and 12 years to become who they are today.
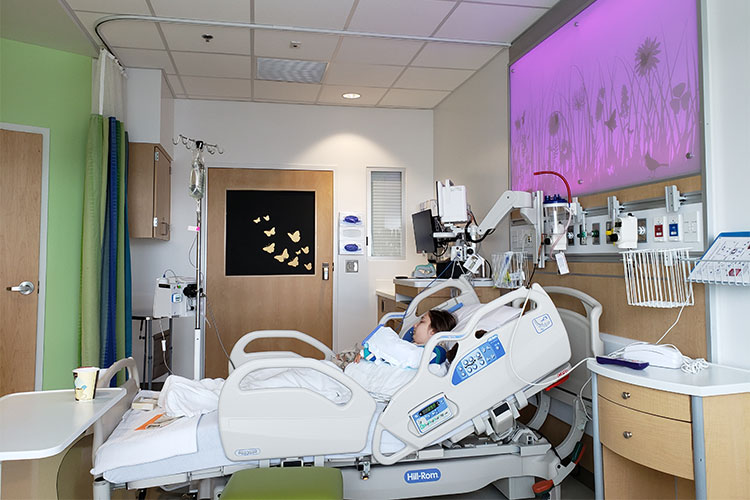
Being on the receiving end of this highly organized model of healthcare delivery really brought home the importance of designing equally dynamic environments: ones that balance formal labs and classrooms with informal “soft” spaces, reading nooks, and collaboration rooms. As architects and planners, we’ve been involved in the design and construction of millions of square feet of medical learning environments for dozens of colleges and universities across the country. While every design is unique, each leverages the following three essential concepts. They’re the keys to creating successful environments for future healthcare professionals to hone their crafts in a collaborative way.
1. Make Simulation As Realistic as Possible

Simulation is about specificity and intention. Students will matriculate to a diverse array of professional organizations and may encounter a wide range of environments throughout their careers. An OR is a very different space from an ICU. Which are utterly unlike a dental or primary care physician office. Designing each of these environments requires very specific application of spatial proportion, materials, equipment, lighting, and utilities.
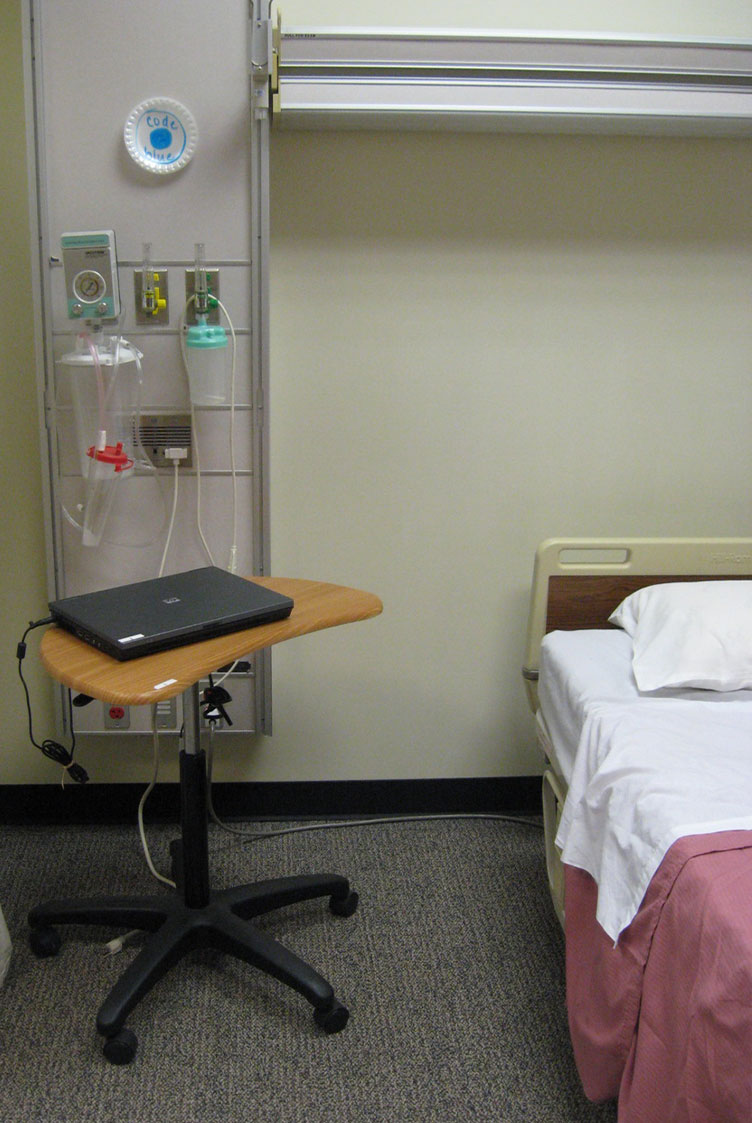
Creating simulated versions of these spaces is no different, but the challenge is the same: removing suspension of disbelief for those experiencing the simulation. The goal is to create a fully immersive environment that is “real”, safe, and provides the opportunity for both collaboration and feedback. We’ve seen our fair share of mock ICU rooms before at accredited colleges where the Code Blue “button” on the wall was a paper plate with blue highlighter coloring…not exactly a fully-immersive environment.
The more immersive, realistic, and functional the environment, the more confident and seamless the transition will be for students from educational to professional realms.
2. Include Emotional Decompression Spaces
Medical education can be intense, emotional, and stressful. Imagine you’re a teenager, and you’ve just run through your first E.R. simulation where a “patient” died. Thankfully, it’s just a simulation — but if I’ve done my job right, that room and experience should feel like the real thing. When that happens, it’s critical for the institution to support the mental health of its students.
Designing “in-between” spaces for decompression are as important to get right as the program spaces themselves — for the social and emotional needs of students (as well as faculty and staff). Nooks and crannies in buildings – places for quiet study, small group activities, or even just a place to cry – are as necessary for a medical student as the large, wide open atria we see in so many facilities today.
A better building is one that can anticipate and provide for a broad spectrum of student needs, through the creation of spaces that are vibrant, healthy, sustainable, technology-enriched, flexible, comfortable, and attractive. The building must actively foster collaboration among its occupants and force interactions that might improve outcomes, research, or educational opportunities.
Design that supports the full range of student needs will result in not only their success, but success for the institutions they attend.

3. Prioritize Occupant Health
Sustainably focused design plays a strong role in enhancing and supporting occupant health. Students that graduate with good physical and mental health enter the workforce with the built-in advantages: higher energy and stronger emotional resiliency, They’re also more likely to promote healthy lifestyles in their patients.
So it’s important to make health-conscious decisions when their learning environments are planned. While passive responses (specifying materials that do not off-gas breathable toxic chemicals, or providing ample access to daylight throughout a facility) are critically important, new building environments must also actively promote the health and well-being of their occupants and users. Buildings need to give students healthy choices: they’re more likely to take stairs if they aren’t dark and scary, like something out of a horror movie; they might skip the vending machine if healthy food options are available.

Why it Matters
When my daughter broke her arms, the closest emergency department happened to be a freestanding facility in suburban Columbus that I helped design. (In fact, the facility itself was a unique model of collaboration between two healthcare providers: Nationwide Children’s Hospital and Ohio Health. It turns out that some of the nurses and doctors she was treated by were educated in facilities I also helped design.
So, as I sat in a patient room I designed, watching my daughter being treated by a team of people who were educated in facilities I also designed, I was glad that I knew I had imbued those facilities with the three principles I listed above. I was glad for the role I played in being a champion for collaborative environments to learn and practice. But above all else, I was glad for the collaborative, coordinated care our family received.

Ben Niebauer, LEED AP BD + C // Associate Principal, Education Market Leader
Ben leads DesignGroup’s education practice. He has focused his 18 year career on exceptional design and planning for academic facilities. Ben has significant experience designing student centered environments including medical education facilities, laboratories, over 5,500 student housing beds, and has assessed and planned over 30 million square feet of higher education campuses. Ben is an active participant with the Society of College and University Planners.
