There has been at least one silver lining to the Covid-19 crisis. Telemedicine treatment for behavioral health patients has been very positive – for patients and practitioners alike.
By: Heather Clark, NCIDQ, EDAC // Interior Designer and Emily Wagner // Project Associate
Despite earlier efforts to stem the tide of coronavirus, it appears the second wave is upon us and will continue to impact our lives for the foreseeable future. Few sectors have been affected more dramatically than healthcare: facilities that weren’t stretched to the breaking point with COVID-19 patients were, ironically, coping with a dramatic drop in elective procedures or non-urgent cases.
One area that needed as little disruption as possible was behavioral health. These patients rely on trusted, ongoing relationships with doctors and counselors in a range of specialties. Fortunately, one (relative) bright spot during this crisis was the industry’s response for these patients. The solution in an age of caution and social distancing? Telemedicine. These virtual sessions performed over computer or telephone provided the continuity of care these patients needed.
In recent weeks, DesignGroup has explored different ways healthcare providers have responded to the pandemic, primarily in terms of facility and operational planning. In this article, we focus less on the physical environment and more on the therapeutic relationship between patient and clinician.
In some ways, behavioral health lends itself better than other specialties to remote treatment. We spoke with clinical psychologist Dr. Doug Henry of Allegheny Health Network (AHN) and psychiatric facility designer Frank Pitts of Architecture+ to better understand the role of telemedicine in behavioral health.
A Sudden Ramp Up
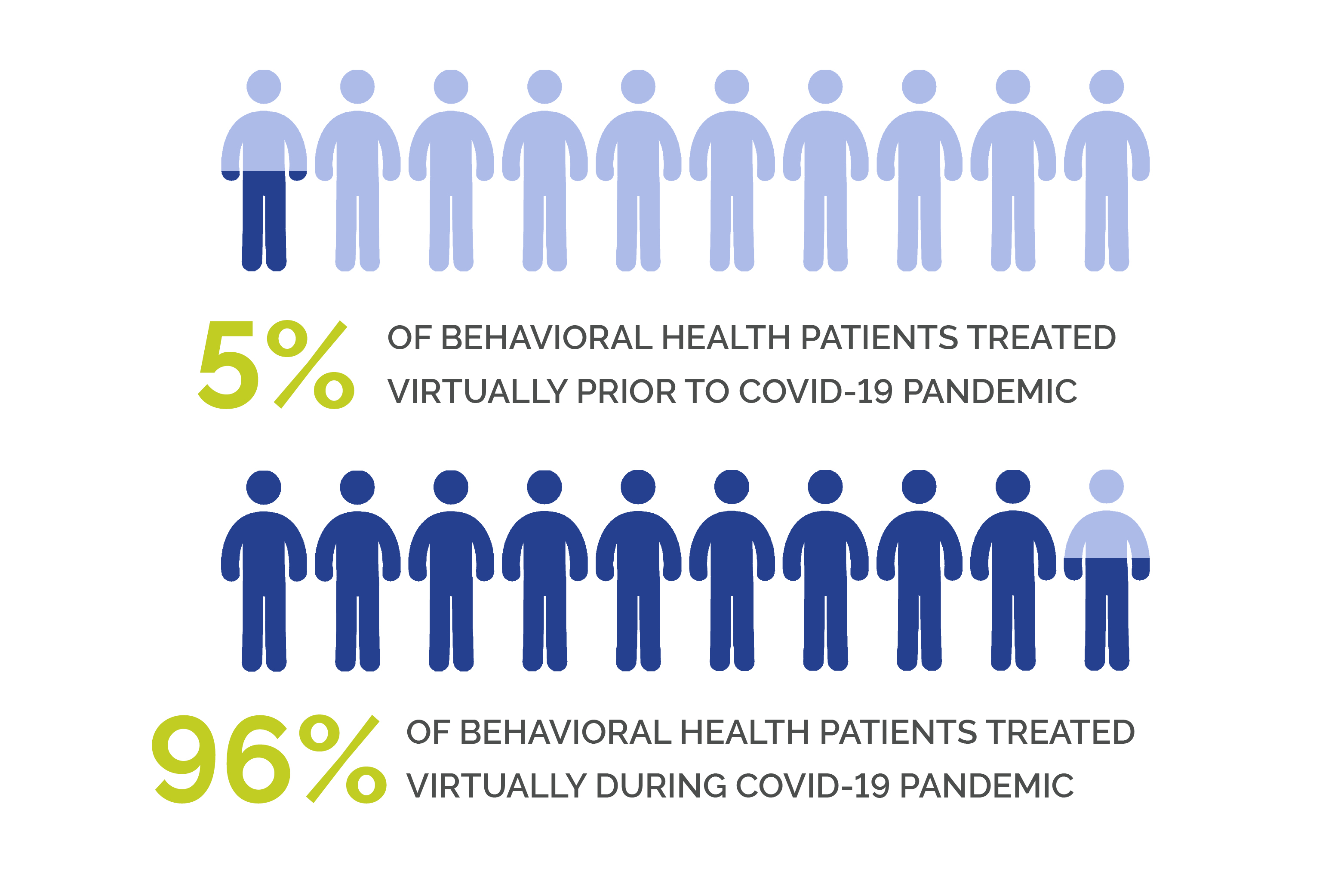
Before the pandemic, a small number of patients were already being treated virtually, so practices were able to scale up quickly. At Allegheny Health Network, within days of the stay-at-home order, virtual visits jumped from 5% of patients to more than 90%.
In fact, Henry says psychiatry and behavioral health services were the only areas of medicine that increased volume during the pandemic. Despite the immediate uncertainty that patients and clinicians faced, both groups reported very positive experiences with remote treatment. “Providers have also benefited from telemedicine and working from home,” Henry says. “Clinicians feel they’re being more productive with the treatment of their patients.”
Another positive that both Henry and Pitts have reported: No-show rates for telemedicine appointments fell by as much as 10-12%, according to AHN statistics. It’s been especially beneficial for lower-income patients, who were unburdened of driving and paying for parking, or relying on public transportation, or finding a babysitter. “Having access to telemedicine from home is a real patient amenity,” says Henry. “When the disruption forced the schools to be closed, that left a gap for students with behavioral health issues that could be treated by a school clinician.” So AHN quickly acquired a grant to secure 60 smartphones so therapists could continue treatment remotely with student patients through a secure telemedicine portal.
Challenges to Treating Patients Remotely
A few exceptions to this high-tech solution exist, of course, primarily with older people and some teens. For older patients, concerns stemmed from less familiarity and comfort with the technology. For teenagers, the problem was just the opposite: they were too familiar with the tech. Many felt uneasy meeting with their clinicians, describing it as “creepy” and too similar to their video chats with friends and others.
The 4% of patients who’ve continued in-person treatment during the crisis have been primarily young children and specific cases where neuropsychological testing was needed. It’s a challenge for clinicians to interact with a child through a webcam and not miss any signs. It was also difficult helping patients with signs of dementia. Many such evaluations were put on hold until they could be safely welcomed back into the office.
Another concern mentioned by Henry and Pitts: the patient’s home environment. Prior to the pandemic, patients were typically treated in the neutral space of a clinician’s office. Now, clinicians must be extra vigilant in ensuring their patients feel safe at home.
The Healing Environment
Even before AHN implemented a telemedicine option for patients, Henry says they relied on a “subtraction” framework to establish a baseline of needed services — by removing components that aren’t essential. Subtraction exercises were useful in determining how telemedicine could deliver the same level of safety and efficacy under trying new circumstances.
Like the surprising success businesses are having with distance workers, some therapists may be asking: If telemedicine works so well, does therapy really need to occur in the clinician’s office? After all, a connection is ultimately defined more by the therapeutic relationship than the physical location. Some clinician offices have interesting stuff hanging on the wall and are warm and inviting. But a great therapist, sitting in a cold, sterile isolation room, can still do great work.
It’s an interesting question, at a time when the pandemic is challenging many assumptions about space and design. And we’re seeing changes already. In the design of AHN’s outpatient centers, redesigns include dedicated telemedicine spaces. There will be three to four “green rooms” which will help further to treat patients remotely. As designers, we’re newly mindful of the layout of such spaces — whether they’re large, open rooms or individual private offices — to be camera-ready and provide opportunities for visual stimuli or other imagery in the background to support a calming, healing environment.
Taking things a step further, Henry challenges us to consider what psychiatric hospitalization would look like without the hospital. Could a patient be hospitalized at home safely? Imagine nurses completing rounds by joining a virtual call every 15 minutes, clicking from room to room instead of walking. Patients would take advantage of local support systems and familial supports within the home. It’s interesting food for thought.
Looking Ahead
Is telemedicine here to stay? Regulatory factors will play a part in the continued use of telemedicine services. Many rules and restrictions for telemedicine were loosened during the pandemic to serve the patient population; institutions will need to lobby for lifting some restrictions for telemedicine appointments to become the new normal. There are also concerns around insurance coverage —providers are not guaranteeing coverage of virtual therapy after specific dates.
Thanks to the resounding success of telemedicine at AHN, the company is advocating with state medical and mental health services, as well as CMS Medicare and Medicaid for the ability to continue to provide services remotely.

Heather Clark, NCIDQ, EDAC // Interior Designer
Heather is a resourceful, accomplished and dedicated interior designer with 23 years of experience in conceptual design, space planning and client leadership with a specialty in healthcare planning and interior design. She is adept in working with colleagues & clients to achieve a shared vision that fosters creativity which delivers results that exceed expectations. Heather is an NCIDQ professional with a strong drive to engage in evidence based design and sustainable design.

Emily Wagner // Project Associate
Emily joined DesignGroup after graduating from Pennsylvania State University with her Bachelor of Architecture. She has a passion for collaboration and enjoys learning new skills and techniques to improve design and the quality of her work. In her time at Penn State, Emily was a member of the CoLab team selected as the jury award winner for best design of a healthcare facility for team collaboration and presentation. Emily studied architecture because of the vast opportunities to create a positive impact on people’s lives through excellent design.
