Every four years, Facility Guidelines Institute (FGI) releases an update. With the rollout of the 2022 FGI Guidelines for Hospitals fast approaching, DesignGroup has broken down key changes and what they mean for facilities moving forward.
By: Angela Kolosky AIA, NCARB, LEED AP BD + C // Associate Principal, Healthcare Planner
While many items have shifted and updated, three progressive topics have surfaced in 2022. Common to these topics is the relationship between departments and how care is delivered, and the needs of clinical staff vs vendors and code requirements. This three-part series will highlight the key areas of changes for 2022 and their impact on design.
Behavioral Health Updates Behavioral health has been among the most talked-about healthcare topics of the last few years. When the 2022 FGI Guidelines go into effect in 2022, the greatest impact in this area will be in the relationship of patient care and other services. Changes have expanded protections for patients by pushing anti-ligature out into the facility, expanding care methods within the emergency department to better care for the wide spectrum of behavioral health conditions, and providing multi-faceted response to patient care without the need for hospitalization.
Mental health affects so many people and, sadly, the system has struggled to keep up. Behavioral health is successful when it avoids one-size-fits-all treatment and meets people where they are. The expanded guidance in FGI 2022 attempts to do just that.
Expanded Protections
Mental and behavioral health patients do not always present to the hospital through the ambulance entrance. They may self-admit or seek other treatment. FGI’s new anti-ligature commentary seeks to expand these protections out of the typical areas, and into new areas such as ED waiting and hospital public toilets.
Timely Intervention
In the wake of the pandemic, EDs have become even more busy in caring for medically ill patients, then adding in behavioral and mental health patients contributes to even more of a backlog. The Behavioral Health Crisis Unit guidelines allow for a specialized space for immediate and extend care needs of patients who do not need medical care. This allows for focused treatment and frees up space within the emergency departments.
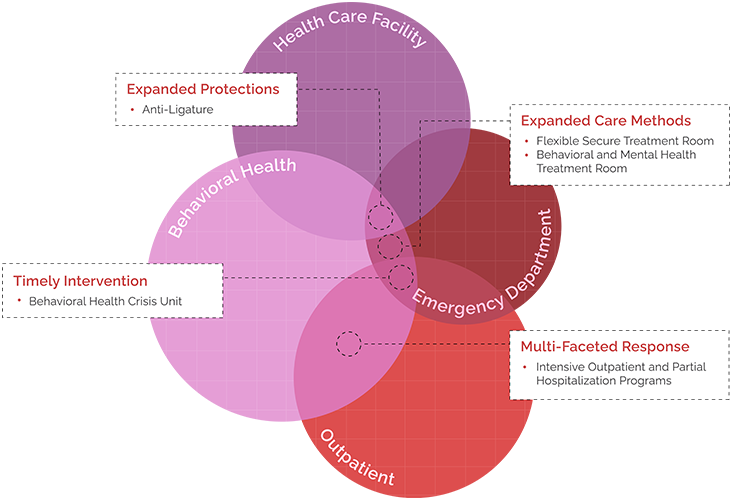
Expanded Care Methods
Behavioral health patients presented to the ED often get placed in a one-size-fits-all treatment space, when in reality mental and behavioral health has an incredibly varied subset of conditions. By providing space that more specifically meet the needs of incoming patients, we can improve their quality of care.
Multi-Faced Response
Just like one room doesn’t fit all for behavioral and mental health patients, neither do standard delivery care models. FGI’s new guidance on programs that bridge the inpatient and outpatient arena allows systems to meet patients where they are.

Angela offers a unique perspective to healthcare planning. Her love for healthcare design stems from her Master’s thesis, “The Importance of Design Decisions in Patient and Staff Outcomes in Ambulatory Infusion Centers,” which focused on how design can create positive outcomes for patients and staff. Angela brings this thinking to every project and has a passion for creating impactful, positive spaces for a critical and vulnerable population. With building performance background data, one can begin to see the impact that initial phases of planning and design have on the end user, which in turn helps healthcare planning and design improve with each new phase or project.
