Blood and marrow transplant (BMT) patients often face an isolated hospital stay that can last weeks. Because they’re highly immune-compromised, they’re often confined to clean environments with little to no physical contact with friends and family. Feelings of loneliness and a lack of control are common — all at a time when their life may hang in the balance.
By Sarah Eversman, NCIDQ, Associate IIDA
Patients aren’t the only ones who struggle with the BMT experience. Families also feel the pain of isolation from their loved ones, and face the same hopes, fears, and frustrations of an unknown outcome. And many hospital staff report that, while their work is deeply fulfilling, it can also be stressful and challenging.
To better understand their needs and potential solutions, DesignGroup took a closer look at typical BMT patients and their treatments – both inpatient and ambulatory – and how design might help lower stress, simplify the experience, and improve outcomes.
In preparation for our work on the OhioHealth Blood and Marrow Transplant Program at OhioHealth Riverside Methodist Hospital and OhioHealth Arthur G.H. Bing, MD, Cancer Center, DesignGroup realized early that all three of these groups — patients, family, and staff — are integral to success, and needed to be factored in design solutions equally. In rethinking the design of a clean healthcare environment, one of our main goals was to shift the patient experience from one that’s cold and clinical to one that provides greater calm, connection, and warmth. In this first of two articles, we focus on the inpatient experience (which can last from 30 to 90 days) and how DesignGroup delivered on this promise. Next month, we’ll look at changes to the ambulatory experience, shorter but crucial visits that happen during recovery.
Mapping the Inpatient Experience
During the design process we met with two individuals, a past BMT patient and a past BMT family member, to understand the patient experience. The discussion was broken down into three parts.
- First, we asked about their mental and physical journey through the facility; their likes and dislikes; which flows were and were not working; and what they wished had been available to them during their treatment.
- Next, we created an experience map to indicate how they were feeling (low stress, medium stress, or high stress) along the path of arrival to departure. Mapping the stress levels of both individuals revealed joy and pain points throughout their journey on a typical day.
- Finally, we were able to share our design visioning, including concepts, goals, color palette, and more with both participants. They were able to confirm that our palette was warm and soothing and that our design concepts followed what they experienced, wanted, and/or expected from a BMT department.
We then concentrated on design solutions to ease the isolation and anxiety that can come with an extended inpatient stay for treatment — often a painful process that can last weeks at a time.
Each person traveling to the BMT inpatient unit at Riverside Hospital, regardless of being a patient or family member, feels fear. Fear of the known and unknown. Fear of the what-ifs, the hows, and the why me. The optimistic thoughts deep inside are often outweighed by the looming diagnosis, treatment, recovery, and their own mortality.
In a perfect world, each new cancer department would be in its own building full of clear wayfinding opportunities, but often the first challenge a patient faces is navigation through an existing facility to the newly renovated space. While we had minimal control over the initial journey from the parking garage to the main entrance to the 6Blue elevators and up to the unit, we could control the journey from the moment the patient stepped off the elevator. This was achieved using three key design strategies incorporated across both BMT projects: calm, connection, and warmth.

Finding Calm Through Color
The look and feel of a calm space can be subjective. Early in the design process our team agreed the use of color, texture, and lighting, as well as gentle tones and grounding elements, were key to creating a more soothing environment for patients, staff, and family. The goal was providing a greater “softness of space” while also adhering to strict healthcare guidelines and air-flow ratios. The first impression of the department occurs in the elevator lobby, where the wall tile mimics the flow of water and a deep-blue accent paint inherent to the healthcare system indicates that you have arrived at your destination. Corridor finishes are simple and clean with accents emphasizing the threshold at patient rooms, while the wood-look sheet flooring exudes a feeling of home. To counter feelings of isolation, the department layout provides opportunities for patients to walk around the entire floor with the triangular, racetrack floor plan.

Connection & Wayfinding
While connection means different things to patients, staff, and families, we drew on commonalities to improve their experiences. Connection to nature is important and has been proven to encourage faster healing. This can be achieved through outdoor views, artwork, and graphics. Another key: providing opportunities for patients to personalize their space, such as dedicated zones to display cards and pictures, and giving them control over lighting. Seeing and talking to friends and family via technology incorporated on the footwall (and easily seen from anywhere in the room), or even a small hand-held device, can go a long way to fighting feelings of isolation. And while each person goes through an individual experience, it is relatable with other patients, so providing opportunities for smaller group connections once the patients have reached a less compromised stage can also help with recovery.
Consistent design and materials for all staff stations help the patient and family recognize “this is where we go for help,” even when they are not aware of the fact. Accent paint used in patient and family zones leads you to a location or marks a threshold and continues inside the space, further connecting patients to their surroundings.

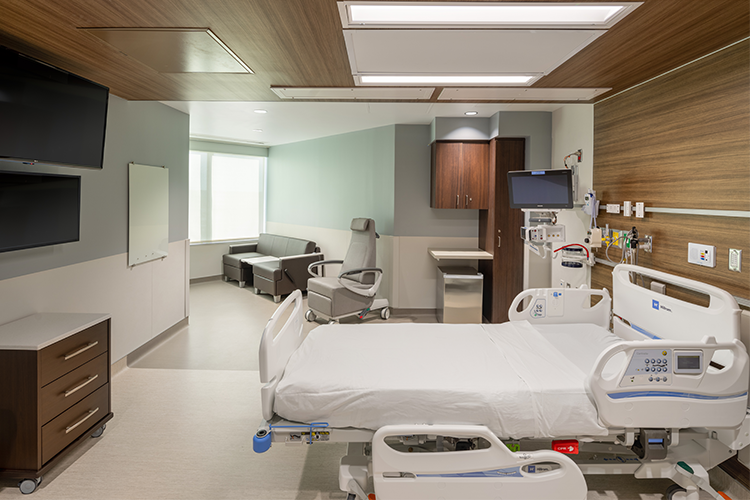
Adding Warmth Through Wood
Incorporating wood elements into a design is the easiest way to bring warmth into a space. We aimed to create a sanctuary for the patient, where they would feel enveloped and safe. Wood wraps the patient from the ceiling and down behind them on the headwall creating a clear patient zone, while a light blue accent paint wraps from the door and around the family seating area. The rich medium blue accent color on soffits above each staff station is further highlighted by the soft glow of a perimeter light fixture. The same accent paint used in patient rooms leads you to the Family Waiting Room with abundant windows and natural light, providing that vital respite needed by all. The kitchenette and island are adjacent to amenities such as a family consult room and laundry room that further provide feelings of home.
Today and Beyond
Our design journey from visioning to patient mapping to concepts to implementation was successful. The inpatient BMT unit is complete and has achieved what we set out to accomplish. The spaces are calm, warm, bright, and inclusive. They provide intuitive wayfinding elements and surround the patients in a gentle and safe environment. Utilizing all opportunities to uplift patients, family and staff is vital in the design process, and while design elements by themselves do not fully heal patients, they play an essential role in the recovery process.

Sarah Eversman, NCIDQ, IIDA
Senior Interior Designer
Sarah brings 17+ years of experience in interior design services for healthcare facilities. Her experience includes working closely with both small and large project teams during ideation and conceptualization through design development and construction documentation. Sarah finds success and value in providing functional, inspiring, and aesthetically pleasing facilities for staff, patients and families and making a positive impact on their well-being.
1 Johns Hopkins, Bone Marrow Transplantation | Johns Hopkins Medicine
