Balancing clinical and family considerations
Neonatal Intensive Care Units are a relatively recent phenomenon in the development of modern healthcare spaces, with the first typically recognized as opening at Yale New Haven Medical Center in 1967. This unit, as with most units prior to 1990, consisted of rooms with multiple infant stations with as many as 20 infants per room. Since the mid 1990’s a greater focus on and understanding of developmental care for neonates has led to smaller groups and ultimately in 1997 to the first NICU with a large proportion of single family rooms.
Creating a Place for Family
The move to single family NICU rooms followed a similar shift in other cohorts of ICU care for adults and pediatrics. The recognition of parent involvement as care partners along with relaxed visiting restrictions has led to a focus on family accommodations within the NICU.
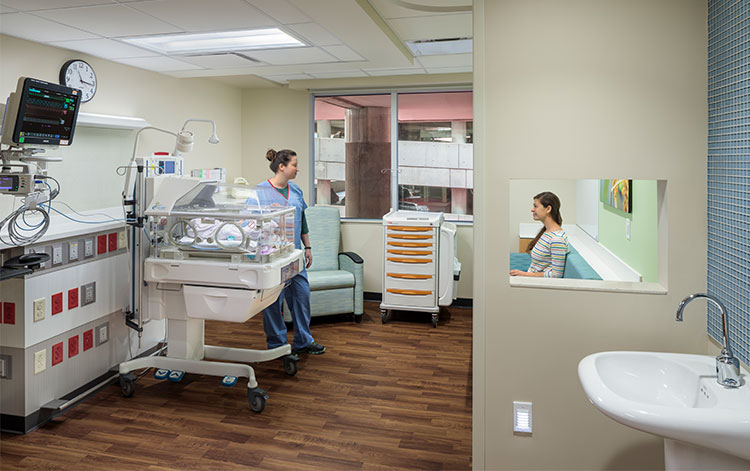
This, coupled with the equipment required to care for high acuity neonates, is continuing to suggest that NICU patient rooms are deserving of the same space allocation and amenities found in other patient rooms within the hospital. The first forays toward individualized spaces resulted in pinwheel configurations that afforded more space and privacy at each bed but still clung to the open room scenario. As the benefits of providing additional area and family accommodation at the bedside become clear NICU’s introduced pods of three-walled bays which helped to balance space requirements with budget. Finally, the leap was made to creating a completely private room environment. This was made possible by new communication and monitoring technology as well as mounting evidence on the benefits of a controlled environment.
NICU rooms are typically equipped with lockable storage for family belongings, sleeping accommodations for one, if not both, parents, breast milk refrigerators and warmers. Some units are also providing private family toilet rooms for each NICU room, although care must be taken to attenuate noise and enhance infection control. Space for parents and siblings needs to be provided outside the patient room areas to support the entire family unit and the transition to home and respite.
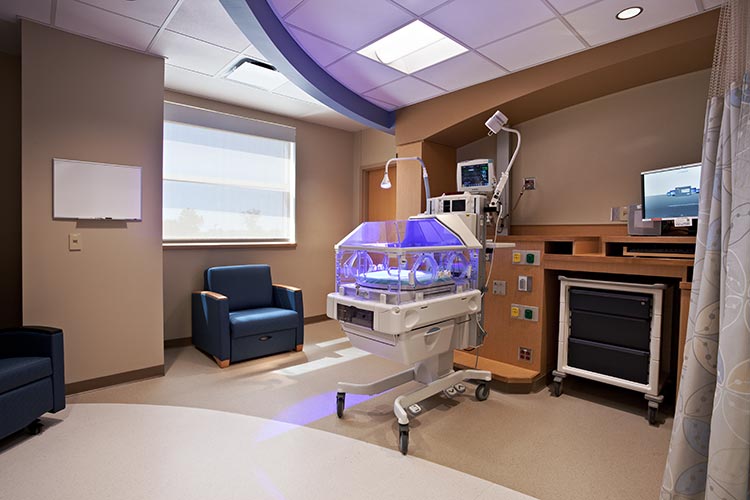
The overall unit is intrinsically changed with the advent of single family room NICU’s. Larger room areas inherently increase travel distances. Therefore, strategies need to be developed to decentralize work areas for nursing staff and the many specialty subconsultants that are involved in the collaborative care of patients in the NICU. Technology has also answered the call with alarm management solutions that eliminate the audio alarms within the unit and notify staff directly when attention is needed. This has extended to adaptations for fire alarm system alternatives that eliminate the need for audio alarms and flashing strobe lights. Many staffing changes studies conclude that nursing ratios can remain similar to those of open units. However, the number of staff needed to support biomedical engineering, environmental services and supply control often increase given the reliance on communications technology, monitors and increase in physical area.

The environment should balance the needs of the family with those of the staff. Staff need ergonomic work spaces at the infant care station with supplies, charting, medication and nourishment resources close at hand. When possible, service personnel should be able to access linen and trash without entering the patient room. Task and room lighting (artificial and natural) can be controlled for each individual patient in the single family room setting and tailored for their developmental needs.
Materials for a Healthy Environment
As designers, we advocate for sensitivity in maintaining a healthy built environment. Sustainable practices are a focus for the NICU for the finishes selection and supplies that are used to support infant care. Materials should be selected that reduce exposure to toxins when looking at anything from IV administration, cleaning products used in the NICU and composition of building materials. Similarly maintenance of heavy rolling equipment such as portable x-ray units can reduce noise by 30 dB by lubricating parts. While organizational and behavioral interventions can be successful, building in noise reduction into the design can be most effective. The design should keep these criteria in mind to allow the transformation of existing environments to state of the art facilities to support the highest level of patient care, family considerations and staff engagement.

Principal, Senior Healthcare Planner
Jane earned her Master of Architecture from Harvard University Graduate School of Design and has dedicated over 27 years to providing medical planning and architectural design services for healthcare organizations throughout the country. Jane is a nationally recognized speaker in NICU and pediatric planning and design. Her most recent NICU presentations have included:
- 5th Annual Developmental Therapists in the NICU Conference (Oct 2010) “Going Green in the NICU: Architecture and Interior Design Elements”
- 14th Annual Children’s Hospital NICU Leadership Forum/Striving for Excellence (April 2010) “Going Green in the NICU”
- NACHRI Annual Conference 2009 (Oct 2009) “A Carefully Calibrated NICU”
- Children’s Hospital Association (previously NACHRI) Creating Connections Conference “Growing Ambulatory Surgery by Reaching Out”
